Dr. Jason Woods’ research focuses on novel ways of imaging lung structure and function with techniques that don’t require sedation, anesthesia, or radiation. The two most promising techniques both use MRI—a modality that uses radio frequencies that are lower in energy than a typical cellular telephone. Lungs have historically been difficult to image with MRI because the blood flowing through the complex capillary bed prevented them from showing smaller lung structures and tissue. These new techniques have changed that significantly.
By using an apparatus on top of the chest, called a “coil,” he can capture the magnetic signal in water and blood contained within the lungs before it deteriorates (very quickly in the lung!). He is able to generate MR images almost as clear as a CT, but without any ionizing radiation. This “UTE MRI” allows subtle structural abnormalities to be visualized and quantified in the lung—sometimes before any functional deficits are apparent in pulmonary function tests.
In a recent study, Dr. Woods and colleagues in the Neonatology and Radiology Departments were able to demonstrate lung abnormalities in the lungs of babies born very prematurely. This imaging occurred in our MRI suite located within the NICU, a system and setup that is unique in the world. This study opens the door to understanding how new treatments affect underlying lung structure and hold potential for further improving our standard of care for these patients.
Another technique that Dr. Woods has pioneered in pediatrics is the use of “hyperpolarized” gases. This allows him to “see breath” and image real-time ventilation in patients with lung abnormalities such as cystic fibrosis or rare lung diseases. These gases (3He or 129Xe) have high-spin magnetism—so they are easily seen on the MRI—and are completely inert (not radioactive). In 10-15 seconds, high-resolution images can be acquired of the entire lung, which holds promise for understanding small abnormalities in regional ventilation—something not possible with traditional pulmonary function tests. In an ongoing study, Dr. Woods is using the combination of UTE and 129Xe MRI to try to understand how small structural abnormalities relate to nearby functional deficits. The hope is that this understanding will better tailor future treatments in individual patients, making personalized medicine a reality.
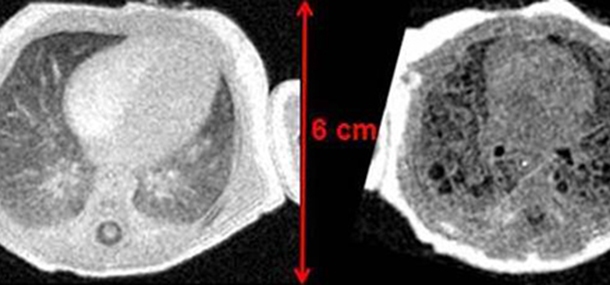
 Image: Normal lung on left and lung with cystic fibrosis on right.
Image: Normal lung on left and lung with cystic fibrosis on right.