Since he was an infant, few things have brought 5-year-old Ephraim Lober more joy than music.
He attended his first  baby music class at just 6 weeks old and was totally enthralled. He quickly became the poster child for music therapy at his original hospital. His providers witnessed firsthand the way it transformed his inpatient days. But when it came to Ephraim’s medical care, there was never any harmony. Only a screeching, shrill cacophony (discord).
baby music class at just 6 weeks old and was totally enthralled. He quickly became the poster child for music therapy at his original hospital. His providers witnessed firsthand the way it transformed his inpatient days. But when it came to Ephraim’s medical care, there was never any harmony. Only a screeching, shrill cacophony (discord).
Born with Three Rare Genetic Disorders
Ephraim was born with three rare genetic disorders, including a duplication at chromosome 2q13 and mutations in the OCRL1 and CACNA1A genes. He has endured a number of medical challenges in his short little life. He was nearly 3 years old before specialists in our hometown identified the full extent of his diagnoses. When they did, they said that there had never been another individual with his particular set of genetic disorders. And statistically, there would never be another. In short, there was no manual on how to treat and care for Ephraim.
2016 and 2017 were incredibly difficult years for Ephraim medically. He was hospitalized monthly with a number of life-threatening signs and symptoms that necessitated continual escalation of intervention. By age 4, he had endured nearly 30 hospitalizations. He was fed continuously by a J-tube, or a feeding tube in his intestines, via a pump that he wore in a backpack. His stomach contents were continuously drained by a second feeding tube, a G-tube in his stomach. He received a nightly IV fluid infusion through his port-a-cath. He also required frequent bladder catheterization during the day, and was dependent upon an indwelling Foley catheter overnight. Daily enemas were administered to treat constipation. He was dependent upon over 39 medication doses per day. And his blood pressure and blood glucose levels were monitored every 4 hours.
Ephraim’s Health Continued to Decline
Despite all these interventions and a care team of nearly 14 specialists that spanned Tennessee (where most of his specialists were located), Ohio (where we saw a few select physicians at Cincinnati Children’s who offered programs or procedures not available at our home hospital), and Texas (where we traveled biannually to see a nationally-renowned dysautonomia team), Ephraim’s health continued to decline significantly. His medical team became gravely concerned about his prognosis. No matter how aggressively we chased them, they feared his disease processes would ultimately outrun us and claim his life.
Transitioning Care To Cincinnati Children’s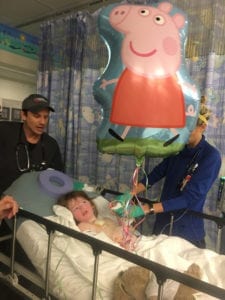
Early 2017 brought two sequential admissions to our local hospital. During these stays, life-threatening medication errors made by staff members placed Ephraim in grave danger due to someone’s negligence. It was time to transition the bulk of Ephraim’s care from our local hospital to Cincinnati Children’s. We retained only our dysautonomia specialists in Houston.
We were floored at every outpatient visit by the help we got at Cincinnati Children’s. They did everything in their power to make our son’s life the very best that it could be. However, they remained respectful of our decision to continue managing his dysautonomia in Houston. They didn’t alter anything related to his treatment for that condition, which had proven to be his biggest nemesis.
Dysautonomia involves dysfunction of the autonomic nervous system. It’s responsible for regulating heart rate, blood pressure, breathing, bladder emptying, gastric emptying, body temperature, and other critical functions.
Ephraim’s Blood Pressure Rises to a Dangerous Level
Fast forward to February 2018. After over a month of blood pressures in the 180s and 190s, Ephraim crossed over the 200 threshold one afternoon. Our son was in imminent danger of stroking out and losing all the cognitive and physical function he’d fought through years of therapies to attain. We were determined to avoid further medication errors and get Ephraim directly to the best care available. So we headed to Cincinnati Children’s emergency department.
Ephraim Loses Consciousness
While his blood pressures stabilized without much intervention, Ephraim pulled another trick. He dropped to the floor in front of the nurses’ station and lost consciousness, pupil responsiveness, and the ability to speak. He was limp like a rag doll, unresponsive and unable to be woken. We had been dealing with these episodes for some time. No one had been able to give us a good answer as to what caused them.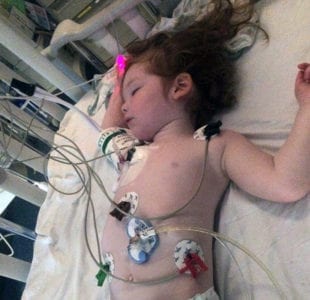
The episodes were terrifying, but his vital signs remained stable during them, so no intervention had been initiated. He’d begin hitting his head rapidly and then quickly lose consciousness. The nurses were horrified by what they witnessed and said that it definitely wasn’t normal. We had the neurology team in our room within minutes, and they ordered a full work up, including a 24-hour EEG and sedated MRI.
When Dr. Franz, his neurologist, met us in the PACU after Ephraim’s MRI to deliver the good news that they hadn’t found any abnormalities, I began to sob hysterically. He was confused: why wasn’t I thrilled by the good news? I wasn’t thrilled because my son had gone unconscious 17 times in the last 24 days and I was so desperate to know WHY and to have a way to fix it. Little did I know that my breakdown would be the beginning of Ephraim’s miracle journey.
The Beginning of Ephraim’s Miracle Journey
When we made it back to the floor, the phenomenal nurses on A4 North questioned what had happened to upset me. I explained my despair over not having a plan to fix this aspect of Ephraim’s presentation. They made a couple of phone calls and within 5 minutes, Dr. Stuart Goldstein, Ephraim’s nephrologist, materialized in our room.
Through my sobs, he heard the desperation in my voice. I desperately wanted to make things better for my baby. We just weren’t getting anywhere with treating Ephraim’s dysautonomia or understanding these unconscious episodes. Ephraim didn’t have these episodes when he was on a specific medication two years ago. We discontinued this medication due to renal side effects. It was clear that Dr. Goldstein CARED deeply, despite it being Friday evening and having other demands on his time. He assured me that we would schedule a collaborative follow-up appointment with himself and Ephraim’s neurologist. At that appointment, we’d discuss options for achieving better control of Ephraim’s blood pressure and helping these episodes to abate.
Hypothesis: Ephraim Was Having Hemiplegic Migraines
A couple of weeks later, I received an email from Dr. Goldstein. He had spent a lot of time thinking about Ephraim and talking with all the members of his team. Rather than the collaborative appointment, he wanted to admit Ephraim to the hospital for a five to six day stay under the direction of the Yellow Team. This was an inpatient team dedicated to overseeing care for medically complex children. His plan was to re-initiate the medication we had discussed while closely monitoring the renal fall out of doing so.
He and Dr. Franz hypothesized that perhaps the episodes of unconsciousness were actually hemiplegic migraines. This is a condition that is highly associated with mutations in CACNA1A, the disorder that this particular medication treated. If their hypothesis were correct, it would explain why Ephraim didn’t have the episodes of unconsciousness while taking this medication previously. It would also explain why no abnormalities had been identified on EEG or MRI. Hemiplegic migraines wouldn’t show up on either of those tests.
He hoped that the medicine might also help to treat Ephraim’s dysautonomia. This may enable us to perhaps decrease the volume of fluids Ephraim received intravenously each night. David and I were on board with the plan but a little terrified. The IV fluid had been the only thing saving Ephraim from constant hospitalization.
Ephraim’s Care Coordinated by the Yellow Team
Ephraim was admitted for the coordinated stay on March 12, 2018. Dr. Goldstein chose a week where several of Ephraim’s key specialists were in house, working together. Early in the stay, Dr. Reddy, his urologist, said that the Yellow Team would act as the conductor, ensuring that each section of the orchestra was doing its job effectively and in conjunction with the other sections. By coordinating care across disciplines and working as a team with the shared goal of improving Ephraim’s quality of life, he believed that they could begin to “make music instead of noise.”
Miraculous is the best way to describe the week. The team initiated therapy with Diamox. As expected, there was some renal fall out. But this was easily managed by increasing the dosages of a couple of his supplements. The team only altered one thing at a time in order to see definitively the impact that each change had. Their goal was to treat the underlying disease process driving much of his clinical presentation. The results of that week surpassed even our most optimistic specialists’ expectations.
Four days in, the team had completely weaned Ephraim from his nightly IV fluids. They expected this process to take months, if it was even feasible. When he was discharged on March 21, he hadn’t had an unconscious episode in six straight days. He was emptying his bladder reliably without any catheterization. The child who had spent years vomiting when he received over 10 mL of liquid into his stomach and sometimes vomited up to twenty times a day even when receiving all nutrition directly to his intestines, was now tolerating 100% of his tube feeding volume into his stomach.
Ephraim’s Health Improves Greatly
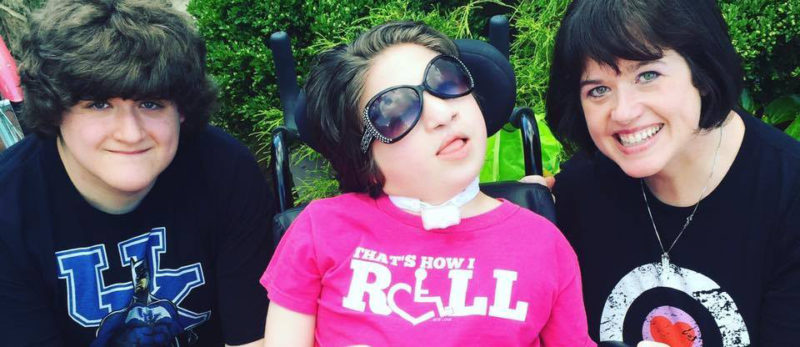
Four months later, the news is even better. Ephraim hasn’t had a single hemiplegic migraine since his discharge from that stay. That means NO unconscious episodes for four months! He is now eating orally during the day for the first time in three years, typically consuming 60% of his daily caloric needs by mouth. Therefore, he is only reliant on his feeding pump overnight.
He wore that backpack for three and a half years and no longer has to wear it. He also now knows what it’s like to enjoy childhood activities like slides and gymnastics without his “turtle shell” interfering.
Ephraim Celebrates His 5th Birthday
 Ephraim turned 5 years old this past May, and what a birthday it was. He enjoyed a birthday dinner for the first time in his five years of life — as well as birthday cake! This did our hearts more good than I can express in words. In fact, this was the first birthday in several years where I didn’t wonder whether it would be the last party I’d get to plan for him.
Ephraim turned 5 years old this past May, and what a birthday it was. He enjoyed a birthday dinner for the first time in his five years of life — as well as birthday cake! This did our hearts more good than I can express in words. In fact, this was the first birthday in several years where I didn’t wonder whether it would be the last party I’d get to plan for him.
Ephraim will continue to face medical and developmental challenges and rely upon supports like therapies, mobility aids, medications, and his feeding tube to thrive. But, going forward, we know, and, most importantly, Ephraim knows, that he will navigate those challenges with the help of the most compassionate, devoted, brilliant, and persistent specialists imaginable.
Ephraim’s Care Is Now A Symphony
Our local hospital made a lot of assumptions (incorrect assumptions at that) about Ephraim, based upon his global developmental delays and diagnoses. At Cincinnati Children’s, they see the Ephraim we see. They recognize a bright, exuberant child who is full of potential, intellectual capability, and the capacity to make a meaningful impact on the world. They don’t treat labels—they treat the child in front of them. While acknowledging his genetic disorders, diagnoses, and obstacles, they refuse to allow those to define our spunky, hilarious, and endlessly loving boy. They see a life worth every ounce of the fight and will make his life the very best it can be.
As a result, he has a comfort level with and a trust in his physicians that we’ve not seen at other medical institutions. We don’t have to choose between receiving superb medical care and having physicians who love our child as their own. At Cincinnati Children’s, we have it all. His care is no longer a cacophony. For the first time in Ephraim’s five years of life, we have a glorious symphony.





As a Pediatric Intensive Care RN, and more importantly, the Grandmother of a medically fragile child, who is now 4 years old; May I add my PRAISE and ADMIRATION to Mackenzie’s assessment of Cincinnati Children’s Hospital, Physicians, nurses, and ALL staff! We had similar experiences with local care at a very reputable facility. There is simply no replacement for the excellence, creativity, and ingenuity of Cincinnati Children’s Hospital. Being a PICU RN, it is obvious to me that Tripp’s (now age 4) quality of life, both now and in the future has been (since age 1) and continues to be dramatically altered by the “GIft” of being cared for by Cincinnati Children’s. We drive from Alabama to CCHMC for his care and are always eager and excited to make the journey!