Eczema is among the most common childhood conditions – it affects 20% of all children – and it can also be one of the most frustrating conditions for families to manage.
Because every child’s eczema is different, finding the right care routine can take some trial and error, but there are some things we know about eczema that can help take the mystery out of treatment.
- Eczema is a chronic, complex inflammatory disorder that often begins in infancy.
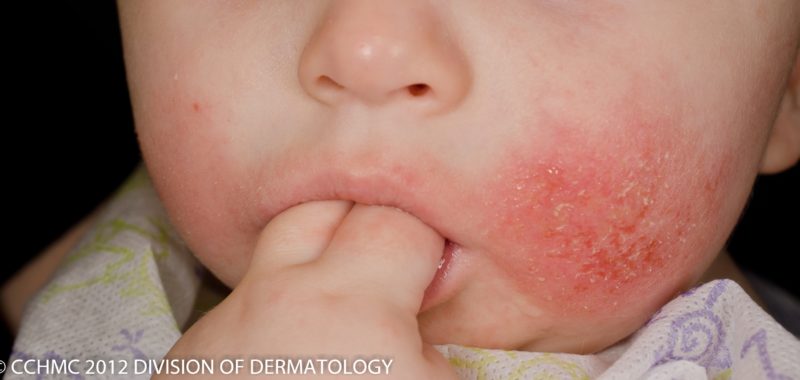
- It results in red, itchy, sometimes painful skin.
- Although any part of the skin can be affected, common areas of involvement include the insides of the elbows and knees, the hands, and the face.
- In most children eczema is not caused by allergies, although eczema, asthma and food and environmental allergies commonly occur together.
- Eczema improves in many, though not all, children by school age.
- The most important aspect of care for children with eczema is a foundation of good skin hygiene (more about that below) and use of medications as appropriate for each individual child.
- Skin infections are common in eczema and may result in flares.
The lack of association of allergies as a cause of eczema was publicized in 2014 when the American Academy of Dermatology released a new position statement which states that there is no significant link between food allergies and eczema – or, stated differently, you cannot “cure” eczema by removing food allergens from the diet. While an elimination diet may be necessary for other reasons, eliminating foods solely for the purpose of treating eczema is not helpful. Eczema and allergies, although often seen together, are two separate entities that require their own evaluation and management.
The basis for eczema treatment is first and foremost good skin hygiene and regular moisturization.
The ideal skin hygiene routine includes daily baths in warm (not hot) water for no more than ten minutes. The skin should be thoroughly cleansed using a gentle non-soap cleanser. For many children daily baths are important for improving skin hydration and minimizing risk of infection. If daily baths seem to make your child’s eczema worse, try bathing less frequently, but keep a particular eye out for any signs of infection.
Moisturizing the skin is the second part of this foundation and it requires regular use and liberal application of a CREAM-based moisturizer. Lotions (oil-in water emulsions that generally come in a pump-type dispenser) are not recommended. The moisturizer should be applied at least 2-4 times per day. For infants and toddlers, it’s easiest to apply it at diaper changes.
The best moisturizer is the one that works for your child. If you have something that you like, there is no need to change products. But for people who need or want something new, we often recommend CeraVe Moisturizing Cream, which has been shown to be superior in research for eczema care. The product contains a protein called ceramide, which works to fill microscopic gaps in the skin and breaks down slowly, providing a “time released” effect. As you’re considering products, please also remember that children with eczema are more likely to develop irritation or allergic reactions to chemical ingredients in skin care products, so avoidance of certain ingredients such as parabens and fragrance may be helpful.
Most caregivers see significant improvement in their child’s eczema within 1-2 weeks after starting a comprehensive skin care routine, but many children may need to use medications to help manage itchiness or flares.
If a child’s rash is particularly itchy, you can keep the moisturizer in the refrigerator – the cool temperature aids in itch relief. A medical provider can also prescribe topical corticosteroids for management of eczema flares, and if you have any concerns about the health of your child’s skin, his or her physician can always help assess the need for medications or a referral to a dermatology specialist. If your child’s quality of life is impacted negatively by their eczema, his or her flares are consistent and severe, or he or she has developed an infection at the site of an eczema rash, evaluation by a dermatology specialist for additional help in managing the condition is recommended.
You can also learn more about our team in dermatology at Cincinnati Children’s and find contact information.





Eczema can be tough for anyone, especially a child. Thank you for providing this great information and helpful tips. They are sure to help out any parent in need!