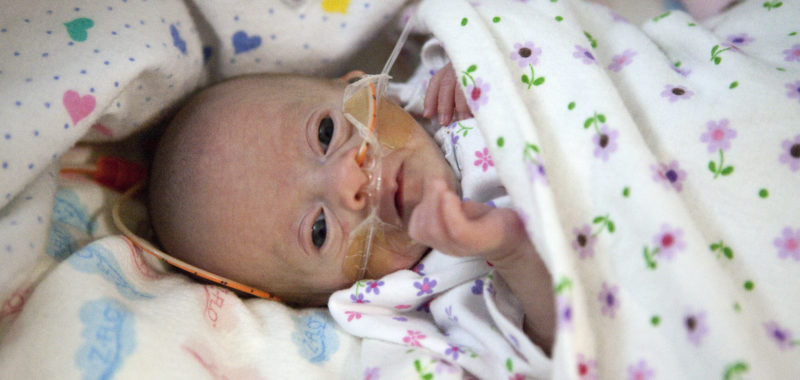
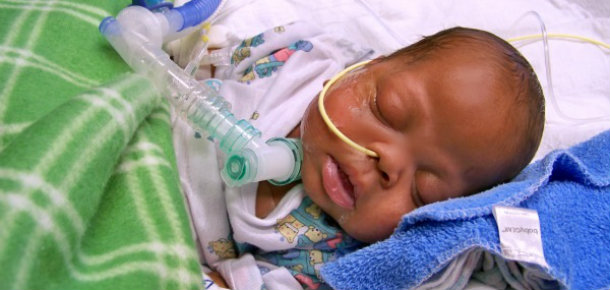
The scientific world has been looking for the causes of preterm birth for decades. Yet it has remained one of the great mysteries of human biology.
We know that preterm birth is a combination of both genetic and environmental factors, and today, the New England Journal of Medicine has published research that provides significant information about those genetic factors.
The study, which was coordinated by Dr. Lou Muglia in our Perinatal Institute, analyzed genetic information and pregnancy data from more than 50,000 women, looking for genetic variations and similarities in women whose babies were born before 37 weeks of pregnancy. The team found six gene areas that are associated with length of pregnancy and the risk of preterm birth – giving them a much more focused roadmap for future research.
Why are genes important?
The environmental factors of early labor and preterm birth are fairly well understood. Smoking, poor nutrition, chronic high blood pressure, diabetes and medical history of multiple miscarriages or previous preterm births all increase a mother’s likelihood of experiencing early labor and preterm birth.
But in more than half of preterm births, none of these factors are present and there is no known cause for the mother to have gone into labor. Doctors call these “spontaneous” preterm births and these are the ones that most likely have a genetic cause.
Unexpected Findings
Three findings from the study stood out as unexpected and particularly important:
- All six of the gene areas identified in this study involve only the mother’s body. It does not appear that the baby’s genes – which are half from the father – play a role in the timing of labor.
- One of the six genes detected in the study strongly suggests that the lining of the uterus plays a driving role in preterm birth. This is significant because it suggests some of the risks may be at play very early in pregnancy, at the time of implantation.
- Another one of the six gene areas points to the possible role of a micronutrient called selenium in a woman’s diet. Selenium, was not previously considered important for a healthy pregnancy.
Can these findings help women who are pregnant now?
No, the significance of this research is that there are now six identified areas where researchers can focus their efforts. Right now, doctors cannot predict which women are at risk. In these six specific areas, scientists will now look for ways to identify women who are at risk for early labor and begin developing ways to intervene if a woman is determined to have one of these genetic variations.
Additionally, doctors associated with this work are not ready to suggest selenium supplements for pregnant women. There is no evidence for it right now. Most people eating a healthy diet get plenty of this mineral. To learn more about selenium, click here for Q&A.
Science Takes a Village
This study has been developing for nearly 15 years and compiling the massive amount of data needed to find these gene areas required years of effort by numerous partners. In addition to Dr. Muglia, work at Cincinnati Children’s was led by Dr. Ge Zhang in our Division of Human Genetics. Most of the genetic data was provided by the company 23andMe, along with similar information from three European nations. The March of Dimes and the Gates Foundation were major funding partners in this work.
In the months and years to come, several of these partners will also be part of this continuing research effort.
More than 15 million babies worldwide are born preterm each year and about one million of them don’t survive. Medical advances have enabled us to provide life-saving intensive care to many babies who wouldn’t have survived just a few decades ago, but some of the smallest, earliest born survivors grow up to face life-long health challenges.
We are confident this newly published research holds significant clues in the mystery of preterm birth and that with this new information, the scientific world will now be able to accelerate the discoveries that will lead to more full-term babies in the future.
Read the full news release. Read the full published paper in the New England Journal of Medicine.